Introduction & History
Kegel exercises are meant to strengthen your pelvic floor musculature, which supports several important pelvic organs, such as the urinary bladder and the uterus. These exercises were developed in by Dr. Arnold H. Kegel, an American gynecologist, in the late 1940’s, as a nonsurgical treatment to prevent urinary incontinence.
Technique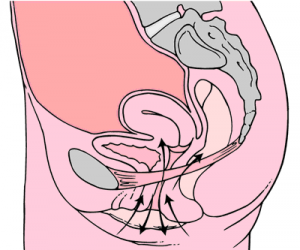
It is very important to “find” the right set of muscles to work on, as many people (one-third of all) perform a Kegel exercise incorrectly, and are actually working their abdominal, buttock, or inner thigh muscles. Therefore, their exercises are ineffective in reaping the benefits of a strengthened pelvic floor.
So how do you locate your pelvic floor muscles? Well, there are several techniques can be used to find the right set of muscles to exercise.
Patients should think of performing the Kegel exercise as if they are trying to avoid passing gas. Women can pretend as if they are tightening their vagina around a tampon. Men should pretend they are trying to stop the urine stream.
Once you’ve identified the right muscles, you’ll feel the contraction more in the back of the pelvic area than the front.
So begin by choosing your position – lay on your back until you get the feel of contracting the pelvic floor muscles. Once you get the knack of it, practice the same while sitting and standing. Contract your pelvic floor muscles for 3 to 5 seconds and then relax for 3 to 5 seconds. Repeat this cycle for 10 times. During this cycle, don’t lift your pelvis and try not to contract your abdominal, leg, or buttock muscles. Place your hand gently on your belly and you’ll feel it if there is any unwanted abdominal action. Then gradually extend the time by increasing the length of contractions and relaxations. Do a variety of short and long “sprints”. Set the goal of doing Kegel exercises several times a day (30 or more) at different times. These can be done anywhere as no one can notice when are doing them.
There are a few emergent settings where Kegel exercises can be performed. If you have stress incontinence, which means that you leak urine when you cough, sneeze, laugh, bend over, or lift something heavy, doing one or more Kegel exercises before some of voluntary events (bending or lifting objects) can help prevent any leakage. Similarly, if you have urge incontinence, which means you leak urine when there is an urge while trying to get to the toilet, doing Kegel exercises may get you safely there. Make sure that you empty your bladder before doing your Kegels.
Kegels in Pregnancy
Pregnant women who perform Kegel exercises are likely to give easier births with less chance of trauma. Having strong pelvic floor muscles during pregnancy can help the pregnant woman to develop the ability to better control pelvic muscles during labor and delivery. Furthermore, it will also minimize two common problems during pregnancy: decreased bladder control and hemorrhoids.
Even after pregnancy, Kegel exercises can promote perineal healing, regain bladder control, and strengthen pelvic floor muscles.
Caution
It is important to do Kegel exercises the right way and one should get guidance from a doctor, nurse or a physiotherapist if needed. If you have pain with these exercises, you should discontinue and see a doctor. If there was a recent trauma or surgery, it is always a good idea to consult your doctor to see if it’s okay to do Kegel exercises and how much.
References:
- https://www.niddk.nih.gov/health-information/urologic-diseases/kegel-exercises
- http://americanpregnancy.org/labor-and-birth/kegel-exercises/
- Effect of home-based Kegel exercises on quality of life in women with stress and mixed urinary incontinence. Cavkaytar S, et al. J Obstet Gynaecol. 2015.
- The status of pelvic floor muscle training for women. Marques A, et al. Can Urol Assoc J. 2010 Dec; 4(6): 419–424.
- Improved continence outcomes with preoperative pelvic floor muscle strengthening exercises.
Sueppel C, et al. Urol Nurs. 2001. - Pelvic Floor Muscle Training: Underutilization in the USA. Lamin E, et al. Curr Urol Rep. 2016.

